
I can’t think of a more awkward social situation for a single, twenty-six-year-old male to be in. A previous experience as the only Jew in a room full of Catholics singing songs about Jesus didn’t hold a candle to this. I was observing a group of fifteen pregnant women discussing pregnancy and getting pregnancy screening tests. Nurse practitioners run this group to aid and educate pregnant women who do not have enough money to pay for individual physician visits or are uninsured or even undocumented. Some of the screening tests, which occur at specified times during pregnancy, include maternal blood pressures and weights, labs to identify low blood counts, tests for sexually transmitted diseases that are a danger both to the mother and the fetus, ultrasounds of the fetus, dopplers of fetal heartbeats, fundal heights (a measurement of the top of the pelvic bone to the top of the uterus) to assess fetal growth, and more.
 |
| Image via Shutterstock |
These tests provide obstetricians with abundant information about the health of the mother and the fetus. For example, a test for gestational diabetes determines whether the pregnant mother may have insulin resistance — a state in which she is unable to store sugar properly, which could cause the fetus to receive excessive sugar and grow too large, resulting in shoulder dystocia, hyperinsulinemia, and hypoglycemia at birth. Screening tests help physicians to identify these sorts of problems early enough to prevent complications.
Obstetricians also examine the cervix, which is the lower part of the uterus. It may be most helpful to think about it as the passageway between the vagina and the uterus. As females progress through childbirth the cervix dilates up to 10 centimeters to allow for passage of the baby from the uterus. The cervix effaces as well; that is, it shortens. Obstetricians check for fetal station, too, an assessment of how far down the fetal head lies in the pelvis — the range is -3 to +3, where +3 indicates imminent birth. They use monitors with probes to assess the fetal heart rate and uterine contractions. The fetal heart rate gives the physician a sense of the baby’s health status. If the baby’s heart slows down too much, the baby lacks oxygen, necessitating immediate delivery.
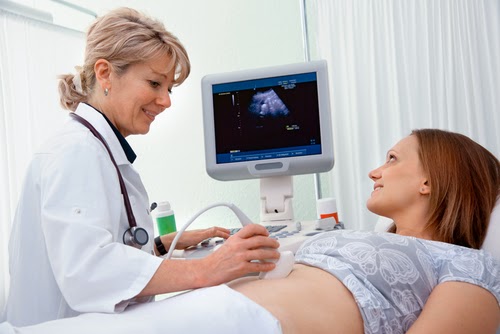 |
| Image via Shutterstock |
The nurse practitioner performed these tests and more for each member of the group over the course of nine months. After some brief screening tests in this particular session, the women sat in a circle and played games. As the only male in the room, I had a difficult time participating in some of these. One game consisted of suggesting an object to bring to the hospital when it was time to have the baby and then listing all the objects the previous patients had come up with — one had to propose something new and remember what others had proposed. Some objects included: a fluffy pillow, baby clothes, a stuffed animal, an R&B CD, a scented candle (cinnamon), and others that I can’t recall. When it came around to being my turn, although I appreciated not being treated as just a fly on the wall I couldn’t help but feel at this moment like a knight in those scenes in Monty Python and the Holy Grail: “Run away! Run away!” I had the eyes of fifteen pregnant women on me. Some of them giggled, either with anticipation or, more likely, because my face turned red and I sheepishly grinned, declaring, “I shouldn’t be here.” I blurted out: “I feel like Arnold Schwarzenegger in Junior.” The reference was lost on every single person in that room; too young, I guess — or too terrible a movie to bother with. So I started to name the objects they had chosen, things that I probably would not take anywhere even if I did own them. I stumbled a bit but managed, with some help, to claw my way through it. When I then had to suggest an object I would bring if I were expecting, I said food. This was met with nods of approval. A love of food is one of those things that certain pregnant women and I share in common.
We next took a short break, during which the conversations mostly covered topics I couldn’t relate to: potential baby names (my only reference for that is this Seinfeld episode but after my previous pop-culture reference fell flat, I knew better than to mention it), pregnancy clothes, car seats, baby clothes, nail polish, and past episodes of morning sickness. I excused myself to “go to the bathroom,” which really meant “avoid the conversations and wander the halls until the break was over.” What else is a twenty-six-year-old male to do in this situation? This was so far removed from any of my experiences or thoughts. After the break, we watched a corny video about the process of giving birth — the acting was so bad that all the actors convinced me that they felt opposite what they claimed to feel. It was a nice time for me to check out mentally.
As ridiculous as this experience seemed at times, there is a deeper, more serious matter worth thinking about here. Many of these women were young enough to be in high school and needed a doctor’s note to excuse them from school. Some of them did not know who the baby’s father was; all except for two were unmarried; and many could not rely on anyone but a single parent for help. Sociologists have thoroughly studied the deleterious effects of these kinds of social situations. As Derek Thompson asserts in The Atlantic:
Among what you might consider “modern families” (e.g. the 61 million people married and living together, both working), there is practically no poverty. None. Among marriages where one person works and the other doesn’t (another 36 million Americans) the poverty rate is just under 10 percent. But take away one parent, and the picture changes rather dramatically. There are 62 million single-parent families in America. Forty-one percent of them (26 million households) don’t have any full-time workers. This is something beyond a wage crisis. It’s a jobs crisis, a participation crisis — and it’s a major driver of our elevated poverty rate.
Indeed, Kay Hymowitz, the William E. Simon Fellow at the Manhattan Institute, writes in the Wall Street Journal that homes without married parents put children “at an enormous disadvantage from the very start of life.” Additionally, teen pregnancy itself causes a range of harmful consequences for both children and their mothers. The National Institutes of Health points out here that teen mothers are more likely to live in poverty, have infants with developmental problems, have baby girls who grow up to be teen mothers and have baby boys who grow up to be arrested and jailed. Furthermore, teen pregnancies have higher rates of illness and death for both the mother and the infant. Though the rates of teen pregnancy are dropping, the problem and its manifestations are evidently very real.
It is difficult to know what exactly the physician’s role should be in this process. How much should physicians encroach on the job of parents, who ought to address this issue with their children? When there are no stable parental figures in a child’s life, how much paternalism does the physician offer? Will such paternalism backfire? At what age is it appropriate to start speaking to teenagers (or preteens) about sexuality, reproduction, and parenting? And what is the best way to do it? Here’s the CDC’s anodyne take on it: “Make your clinic teen-friendly. Provide your adolescent patients with confidential, private, respectful and culturally competent services, convenient office hours, and complete information.” It’s not that easy, nor is it that benign.
The medical profession is unusual in that the private lives of patients are relevant to nearly every visit. Consequently, no matter how uncomfortable or awkward or humorous it may be for physicians, these issues inevitably come up. Undoubtedly, then, medical practitioners will play a role in this deeply significant sociological quandary — how large that role is depends on the physician and the specialty.

Aaron, I will challenge you to embrace your 26 year old male self and to be the one who stays in the room during break, who listens, who embraces a different perspective. That can be scary and feel awkward, but it can also lead to a lot of learning and growth